Loss of muscle mass is often blamed on aging, but in some cases, the real issue involves neurological causes of muscle weakness that disrupt how nerves communicate with muscle tissue.
When that signal pathway breaks down, strength fades, muscles shrink, and everyday movements become unreliable.
One leg may look smaller than the other. Grip strength may decline without explanation. Fatigue sets in faster than it used to.
Not all muscle loss is due to inactivity. Sometimes the nervous system is involved, and knowing the difference can change what happens next.
Let’s walk through when muscle weakness may be neurological, what conditions can cause it, and how it’s evaluated.
Loss of muscle mass, also called muscle atrophy, means muscle tissue becomes thinner and weaker. It can develop slowly from inactivity, poor nutrition, or aging. That’s called disuse atrophy.
Neurogenic atrophy is different. It happens when nerves fail to properly stimulate the muscle. Without regular nerve input, muscle fibers shrink. The process can move faster and may affect one side of the body more than the other.
That uneven pattern is often the first clue that something neurological may be happening.
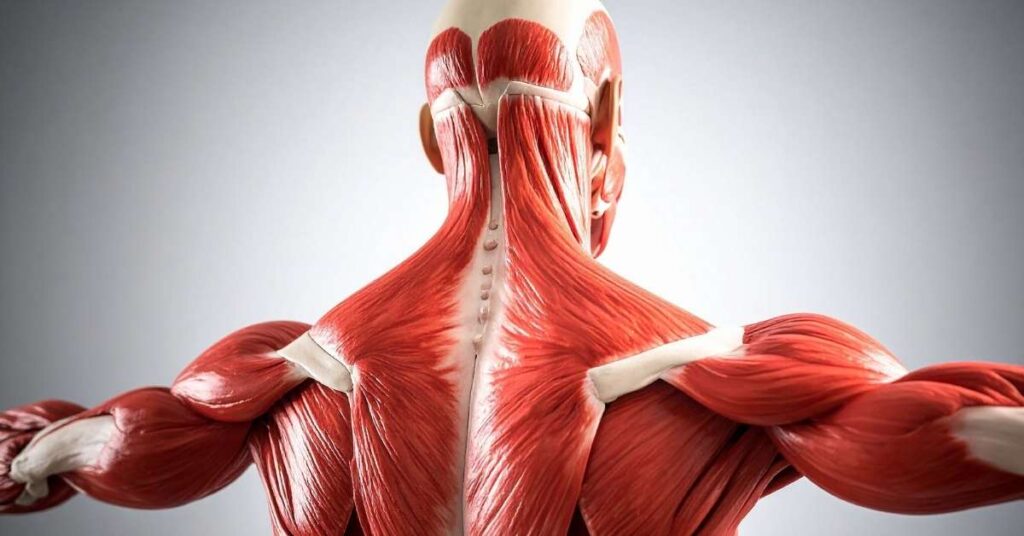
Muscle movement depends on a chain of communication.
The brain sends signals down the spinal cord. Those signals travel through peripheral nerves. At the neuromuscular junction, the nerve releases chemical messengers that trigger muscle contraction.
If any part of that pathway is disrupted, it can be the brain, spinal cord, nerve root, peripheral nerve, neuromuscular junction, or muscle fiber, and weakness follows.
Over time, reduced activation leads to visible loss of muscle mass.
The pattern of weakness often reveals where the breakdown is occurring.
Different conditions affect different parts of the system. The symptoms may overlap, but the underlying cause can vary significantly.
Peripheral neuropathy affects the nerves outside the brain and spinal cord. Diabetes is one of the most common causes. Autoimmune disorders, toxin exposure, infections, and inherited conditions like Charcot-Marie-Tooth disease can also contribute.
Symptoms often begin in the feet or hands and may include numbness, tingling, burning pain, and weakness. Over time, muscles in those areas may shrink due to reduced nerve signaling.
Motor neuron diseases such as amyotrophic lateral sclerosis (ALS) and spinal muscular atrophy affect the nerve cells responsible for voluntary movement.
When motor neurons deteriorate, muscles lose direct input. Weakness progresses. Muscle wasting becomes more noticeable. Twitching or cramping may occur as the remaining motor units struggle to compensate.
A herniated disc or spinal degeneration can compress a nerve root. If that nerve carries motor fibers, the muscle it supplies may weaken.
This often presents as hand pain, sometimes in a specific region, for example, the calf, shoulder, or calf pain, and sometimes accompanied by radiating pain. If compression continues, loss of muscle mass can develop in that distribution.
The neuromuscular junction is the point where nerve and muscle communicate. Conditions such as myasthenia gravis interfere with that communication.
Weakness may fluctuate and worsen with repeated use. Drooping eyelids, difficulty swallowing, and speech changes can appear early. Muscle wasting may develop over time if weakness persists.
Some conditions affect the muscle fibers directly rather than the nerves that control them. Muscular dystrophy is one of the clearest examples.
According to Johns Hopkins Medicine, muscular dystrophy refers to a group of inherited diseases that cause progressive muscle weakness and muscle tissue wasting. Different types vary in age of onset, the muscles involved, and the rate of progression.
Duchenne muscular dystrophy, the most common form, typically begins in early childhood and primarily affects boys.
Becker muscular dystrophy follows a similar pattern but progresses more slowly.
Other forms, including limb-girdle, facioscapulohumeral, myotonic, and oculopharyngeal muscular dystrophy, affect different muscle groups and may appear later in life.
These conditions demonstrate how genetic and neuromuscular disorders can directly impair muscle structure, leading to progressive loss of muscle mass over time.
Inflammatory muscle diseases such as polymyositis and dermatomyositis also fall into this category. In these cases, the immune system attacks muscle tissue, leading to weakness and gradual atrophy.

Evaluation begins with a detailed neurological examination assessing strength, reflexes, coordination, and sensation.
If nerve involvement is suspected, diagnostic testing helps clarify the site of the disruption. Electromyography (EMG) and nerve conduction studies (NCV) measure how well electrical signals travel from nerve to muscle and can distinguish between nerve-related and primary muscle causes of weakness.
Additional testing may include blood tests to screen for autoimmune or metabolic disorders, as well as brain or spine imaging if structural causes are suspected.
In more complex cases, a neuromuscular evaluation may also involve autonomic testing, cognitive assessment, or functional balance testing to determine whether broader nervous system involvement is contributing to symptoms.
Identifying the exact source of weakness allows treatment to be tailored rather than generalized.
If loss of muscle mass is happening without a clear reason, especially if it’s uneven, progressive, or paired with numbness, twitching, or balance changes. Don’t wait it out. Muscle weakness tied to nerve dysfunction tends to worsen when the cause isn’t identified early.
At Universal Neurological Care, evaluation goes beyond a basic strength check. Neuromuscular assessment may include electromyography (EMG/NCV) testing to assess nerve-muscle communication, along with targeted neurological exams and additional diagnostic studies when needed.
Yes. When nerves fail to properly stimulate a muscle, the muscle can shrink over time. This is called neurogenic atrophy and can progress if the underlying nerve issue isn’t addressed.
It depends on the cause. Muscle loss from temporary nerve compression may improve with treatment. Progressive nerve diseases may require long-term management rather than reversal.
Doctors use a neurological exam, along with tests such as EMG and nerve conduction studies, to determine whether weakness is due to nerve dysfunction or to the muscle itself.




